AREAS OF IMPACT
STUDIO
How might we redesign and improve the counselling experience for adolescent girls to create greater awareness about sexually transmitted infections in an HIV-ravaged area of Mozambique?
This important question was at the heart of a project carried out by ThinkPlace for Population Services International that has been recognised with a major design award from New York based Core77.
The project – “Not only informed. Confident” – won a Notable Award from the design magazine.

The challenge
Situated in Southwest Mozambique, Gaza Province is known for two things: extensive cereal and rice cultivation, and its high HIV prevalence.
Around one quarter of the adult population is HIV-positive. Among adolescents, Gaza also sees high rates of unplanned and early pregnancy.
Public and private clinics provide family planning services for adolescents, however, these services are often not perceived as desirable or useful. Due to previous de-stigmatisation campaigns focused on HIV, many people in Gaza proclaim: “Malaria can kill you. HIV won’t.” Many perceive the risk of contracting HIV as plausible for others but not for them.
Adolescents sometimes conflate products which prevent HIV with those that prevent conception, or relate the risk of contracting HIV to the risk of getting pregnant. Condom use is rarely prioritised, especially when it comes to married young women.
There is clear need for access to quality information about these matters. But when adolescents and young women enter health facilities, healthcare workers find themselves providing information that our research showed as often ineffective.
Too often, we see health sector interventions privilege technical, product-focused information over a more straight-forward message that allows the user to actually understand the product, see value in it, and feel confident in choosing it.
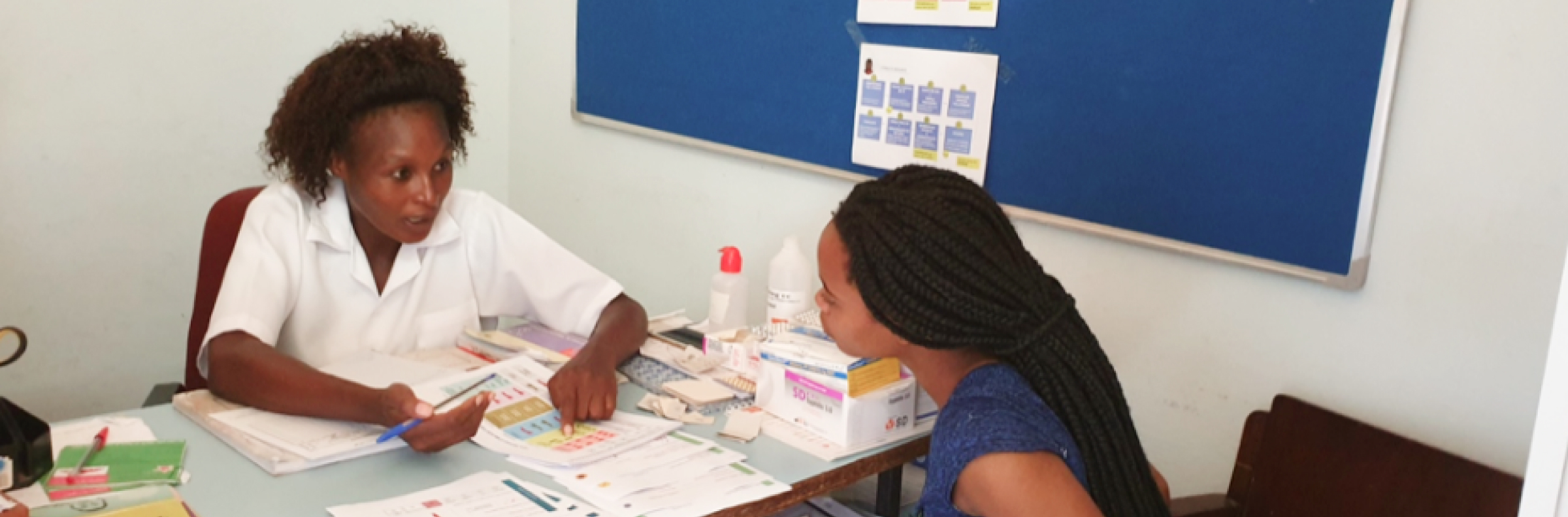
Our response
ThinkPlace worked in five public clinics and three private clinics in Gaza to address the challenge of improving the counselling experience for adolescent girls and young women.
We spent a month in these clinical contexts, identifying the areas where provider behaviour translated to poor patient experience and how that poor experience led to ill-informed decision-making.
To understand the process we immersed ourselves in it. Our team experienced the end-to-end counselling process, like any other patient.
We waited, often for an hour or more, on wooden benches outside each clinic. Once called inside a small, hot, windowless room, a healthcare provider would furiously flip through a script of more than 50 pages, providing a wealth of information about all available contraceptive methods, their side effects and more. Patients were asked to constantly repeat the information and to nod as a sign of confirmation.
According to providers, “If you repeat the information enough, they’ll get it.” But while the information was detailed and informative, few patients left feeling informed.
On average, consultations with first-time users would last for 45 minutes. Patients were inundated with information that did not take into account their lifestyle, their preferences or their specific concerns.
On average, consultations for second-time or repeat users would last for a period of 15 minutes.
This was primarily due to the provider not recognizing the patient’s need to be counselled through a decision around potentially shifting methods. These patients had often experienced adverse effects (e.g. pain, weight gain) and were in need of clarity, reassurance, and advice.
What this four-week immersion revealed to us was not that healthcare providers lacked knowledge about the methods (as is typically the assumption), but that there was no clear intent in how that knowledge was being transferred, translated and adapted to suit the needs of the patient.

How we did it
While this project focused on improving patient experience, we realised through our research that the necessary chain reaction starts with behaviour change on the part of the healthcare provider.
We invited providers and patients to act as designers, holding ‘co-design’ sessions where we worked closely together to identify clear opportunities for change. These opportunities led to ideas for potential solutions, developed into low-cost prototypes, that could be tested in-situ.
Our insights led us to three primary points of intervention:
- the pre-counseling experience
- the counseling experience (for both new-users and repeat patients)
- the moment a patient decides which method to take up.
For pre-counseling, we wanted to isolate the concept of risk. Risk (of contracting HIV, of unplanned conception) is an abstract concept that was often difficult for patients to comprehend. Risk is also subject to bias and perception, leading patients to assess their risk level subjectively.
We worked closely with providers to design a process for helping adolescent girls and young women better understand risk during pre-counselling.
Once in the consultation room, we introduced a revised version of the 50-page script that the providers were using. We asked healthcare providers to help eliminate all information which was not useful or relevant. They eliminated 35 pages.
The revision was referred to as the Minha Escolha (“My Choice”) booklet, which provided information in a highly visual, easy-to-consume format. This information was also visualised through personas and visual pathways that the provider could follow, noting when to ask specific follow-up questions, when to pause and allow her to provide more information.
At the point where a patient decides on her contraceptive method, we asked providers to begin congratulating and celebrating that moment with each patient. We found that this gave girls a sense of not only affirmation but also confidence that they had made the right decision.
The impact
Choosing a method is about the patient feeling like she’s done something to protect herself and that she took control of this aspect of her life. While she chooses it, she can also stay informed about reversing it, changing it, and interrogating it for as long as she likes. And she can do this alongside a genuine ally, who understands her specific experiences, preferences and needs, and advises accordingly.
The Minha Escolha (“My Choice”) booklet has been finalized and distributed and has led to shorter, more fulfilling consultations for adolescent girls and young women.
Before this project, consultations with first-time users lasted about 45 minutes on average. With the booklet, the poster, the pre-counseling interventions, and the congratulatory moment, such consultations are now lasting 25 minutes.
Providers now only share tailored information after listening to patients’ questions and concerns. Before this project, consultations with repeat or second-time users lasted 5 minutes on average. This is because very little consultation was offered to the patient, as providers mostly insisted that any side effects or concerns were “normal” and the patient continued on as usual. Today, those same consultations last 15 minutes on average, as providers offer practical information and guide patients through a change of method should they need it.
On our most recent visit to these clinics, we observed five girls visit the public healthcare facility to get general medical services. The following day, providers were happily surprised to see the same five girls return to the facility and two of those girls had brought a friend with them. It was clear to us how much the clinic had created value for these girls, as they and their peers were craving accurate and clear information about their health.
So we are thrilled that our work has been honoured with a Notable award at the Core77 Design Awards.